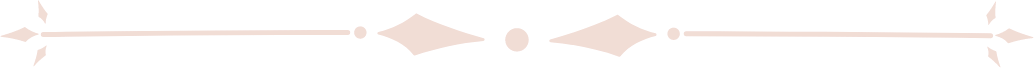Sarah Bell-Booth is a wife and a mother of three lovely energetic children including twins. Her body appears to be preoccupied with ‘multiples’ - with her multiple births and her recent diagnosis of multiple sclerosis. Both of these were a shock, but she has developed resilience to manage parenting while dealing with a chronic illness.
Sarah is also a clinical psychologist who works in private practice. She currently specialises in treating anxiety and depression, particularly in mothers. Sarah is passionate about connecting with those who feel vulnerable and also enjoys creative well-being projects. This has culminated in self-help books, journals and courses to further help adults and children to build their toolbox of coping strategies.
Read Sarah's courageous story below.
I was diagnosed with relapse-remitting Multiple Sclerosis (MS) in 2016. At the time, I was 32 years old, my twins were a year old, and my daughter was three years old. MS is a condition where your own immune system attacks the brain and spinal cord and leaves lesions. These lesions are like holes in the insulation around an electrical wire. They interfere with the transmission of messages from the brain to the body. MS is more prevalent in women and the peak onset is 30 years old– not ideal for child-bearing age. Like some other autoimmune conditions, symptoms usually exacerbate in the postnatal period when your immune system goes on overdrive again after taking a break during pregnancy (so it wouldn’t reject the baby).
The first symptoms I experienced were numbness in my arms and tingly hands. This made my writing on the therapy board shaky and almost illegible (if that’s even possible). I then had unbalanced mobility with mild ‘drop-foot’, like I was dragging one foot along the ground. I looked a bit drunk when walking and I felt buzzing electric-shock sensations down my spine and legs.
“This was extremely hard as a parent. Suddenly I couldn’t push the twin pram up the hill or easily carry my twin babies up the stairs, and I once got stuck on a pebble beach as my legs felt too heavy to move properly.”
This was extremely hard as a parent. Suddenly I couldn’t push the twin pram up the hill or easily carry my twin babies up the stairs, and I once got stuck on a pebble beach as my legs felt too heavy to move properly. I used to walk back and forth across the lounge room to ‘test’ out my walking style. I tried to seek reassurance from my husband by repetitively asking, “am I walking normally now? … now? … how about now?”; He always replied, “no!”. My sweet observant daughter also noticed my walking style and asking if I wanted a piggyback - wouldn’t that be a sight!
Sarah and her newborn twin boys.
In addition, I experienced dizziness, especially in heat. Family members and friends had fun throwing bottles of water over my head or hosing me down fully clothed if I felt faint. My best tips were drinking slushies and wearing a cooling towel – everywhere (it strangely looked like I had just done a workout at all hours of the day). At least the kids scored a portable pool out of my heat intolerance!
Throughout this time, I was hypersensitive to touch. When the kids hugged me or even slightly brushed up against me I would experience a full shiver down my body. You can imagine the intense tickle wars! I also had spasticity (prolonged muscle contraction) and restless leg syndrome, which is the uncomfortable urge to keep moving my legs – almost like a disco party in my legs all through the night. This led to sleep deprivation, exhaustion, and therefore low mood.
One of the most difficult and long-lasting symptoms has been neurofatigue. Sometimes it felt like I could barely keep my eyes open during the day – like the extreme tiredness you experience from jet-lag and the flu, but combined. Even a trip to the supermarket would mean that I’d need a nap before and after. When camping, you could find me sleeping under a trestle table under the shelter. I soon developed a ‘fear of commitment’, as I would frequently make plans then need to cancel due to my symptoms. I hated being unreliable and letting others down.
As an added bonus (and to be honest and transparent in case others experience this MS symptom), I started experiencing urinary incontinence. When I had my first accident, my three small kids couldn’t understand why we drove to the library but never got out of the car! Afterwards, I remember calling my husband crying with a quiver in my voice, “something is seriously wrong – I can’t feel a thing and have lost control”. So awkward and scary contemplating adult diapers at such a young age! This was a huge sign that I needed to check my basic brain/spinal cord function - urgently.
“I didn’t know what the prognosis would be! Wheelchair? Early morbidity? Catastrophic scenarios ran through my mind. My over-researching on ‘Dr Google’ spiralled in a desperate attempt to manage uncertainty. ”
All of these symptoms felt debilitating and overwhelmingly scary. Having had some clinical neuropsychology training, I already suspected MS. Brain health is important for everyone, but I certainly took mine for granted until then. I had only ever experienced temporary illness and now I was facing chronic, life-long issues. I didn’t know what the prognosis would be! Wheelchair? Early morbidity? Catastrophic scenarios ran through my mind. My over-researching on ‘Dr Google’ spiralled in a desperate attempt to manage uncertainty.
An urgent MRI showed both current and old MS lesions in my brain and spine – they looked like bright starry lights on the images. It was strange to wonder how long I had MS without awareness – possibly right back to teenage days when I felt huge bouts of tiredness and couldn’t party all night like my friends without sleeping for a week afterwards. Unfortunately, I needed to wait for another ‘clinical relapse’ before I qualified for funded disease-modifying medication, which would otherwise cost over $40,000 per year for the rest of my life. It seemed so unfair that I had to prove my disability further.
It ended up being a three-year nervous wait before I relapsed. Each day, I would wake up and check I wasn’t paralysed or blind. Although these concerns may sound dramatic, sudden changes are not uncommon in MS. It was a relief to finally identify new, subtle symptoms, and the subsequent MRI indicated new brain and spine lesions. My neurologist congratulated me for being approved to receive monthly immunosuppressant infusions at the hospital. These infusions have been a game-changer. My annual MRIs have shown significant recovery. I feel like I have my energy, and with it my life, back! Despite this positivity, every drive to the hospital is confronting because it reminds me that I still do have this chronic condition and I will need this medication for the rest of my life . It is not quite what I expected my parenting journey to include.
“Mummy has little holes in her brain (said in a light jovial way), but the magic medicine is helping to fix them and give her more energy.”
Over time, my children have started to understand more about what has been going on for their Mum. Initially they got a simplified explanation about MS such as “Mummy just has tired legs and needs lots of naps like you”. Then, “Mummy has little holes in her brain (said in a light jovial way), but the magic medicine is helping to fix them and give her more energy”. Now they are a bit older, my daughter can label it as “MS”. It is not always easy for them to comprehend, but I try to keep it positive. It certainly encourages compassion and caring behaviour in my kids. For example, my little twins used to lay out my ‘day nap equipment’ (big cushion and pillow) on the carpet and quietly watch TV, letting me nap next to them until my alarm would go off after 10-20mins. I am lucky that they are such patient and loving kids.
Sarah with her husband and three children.
LESSONS FROM MY ADJUSTMENT
In the six years since diagnosis, I have used every bit of my emotional resilience and clinical psychology knowledge to cope with the adjustment to this chronic condition.
Here are some of the lessons I have learnt from managing a chronic illness while parenting - both of which have felt uncontrollable and unpredictable at times.
Accepting Vulnerability and Invincibility
Firstly, I have adjusted to the oscillating cycle between feeling vulnerable and invincible. My vulnerability relates to a new world view, considering how precious life is and the importance of health and safety. This vulnerability is activated again when facing new non-MS health issues, like fracturing my ankle or preparing for Covid-19. At times, my mind is hypervigilant to signs of danger, leading to urges to be overprotective of my children. Using my cognitive-behavioural therapy (CBT) skills, I have challenged these excessive fears to maintain a more balanced approach.
Paradoxically, I also feel invincible when I reflect on my body’s ability to effectively bounce back from acute MS attacks. I attribute this progress to modern medicine, as well as my positive lifestyle changes that led to symptom improvement, even pre-infusions. At this time, my neurologist praised me for being a “master healer” and said, “keep doing what you are doing”. This confidence has encouraged me to try new riskier, spontaneous, and adventurous things, such as ziplining, mountain biking, and jumping off a (little) cliff into the river. Freedom!
Tolerating Uncertainty
A major psychological challenge has been tolerating uncertainty about the future. This uncertainty relates to my mobility, my cognitive functioning, and my ability to carry out my various roles as a mother, wife and psychologist. However, I have built up the belief in my ability to cope with the unexpected. I have evidence to show that I am capable.
Accepting uncertainty allows me to be more present-focused and feel excitement in the anticipation of events (sometimes the best part!). This is a stark contrast to dwelling on the negative “what-if” catastrophic thoughts about what could go wrong if my health deteriorated. I am also trying to model this level of acceptance about the future (“you can cope with hard things / you will find a way through”) with my children when they worry about hypothetical events.
Focusing on the Controllable
Focusing on everything I can control has helped throughout my journey. I prioritise quality time with loved ones and choose exercise that I enjoy, including sunrise beach walks and dance classes. I also use relaxation strategies to calm my overstimulated mind, and I try to eat healthy nutritious food (I do love chocolate though!).
Opening a clinical psychology private practice to follow my passion of helping mothers who suffer from anxiety and depression has also helped me. Being self-employed, I have the flexibility to choose part-time hours. I am adaptable and leave a buffer for those extra unexpected events or symptoms. Returning to work has been a gradual process, requiring patience. I try not to compare myself with other psychologists who have larger caseloads and can see double the number of clients in a day, without breaks. I am sticking to my own lane, which sometimes includes some “long blinks” (aka micro naps).
Simplifying Life
Rather than getting caught up in the rat-race of modern society, I try to live a slower-paced lifestyle. Simplifying life reduces stress and fatigue, which would otherwise exacerbate MS symptoms. As is common in my generation, I had a fear of missing out (“FOMO”) on fun, and I previously thrived on keeping busy and productive. However, pacing without overcommitting has been important. I now assertively set boundaries and say ‘no’. In fact, I have been forced to say no to career-advancing opportunities like media and speaking events, cancel pre-registered running events, and pull out of social events. I’m constantly experimenting and learning my limits. Sometimes I accidentally go past my limits, but I try to learn and use self-compassion.
Trusting my Judgement
Another lesson has been to trust my judgement about bodily symptom changes, and advocate for myself with health professionals. I monitor my symptoms and listen to my body. When my body needs rest, I rest – proper restoration without mental stimulation or technology. 1.30pm was my scheduled daily nap, and it would be prioritised like an important meeting.
I also trust my judgment when unhelpful thoughts arise. I can identify negative predictions, self-judgements about being “lazy”, and “should” statements about the need for productivity. I can see my mind is trying to protect, prepare, and motivate me. However, I challenge these maladaptive thinking habits and listen to my gut instincts that are aligned with my values.
Accepting Social Support
I’m continuing to learn when to ask for and accept help from others. In particular, sharing the physical and mental load with my supportive husband has played a pivotal role in my recovery. Being fiercely independent while juggling three young kids and a chronic health condition is impossible (trust me, I’ve tried!). I am grateful for loyal family and friends who remind me of this. When interacting with them, I am honest and express vulnerability when asked how I am; the superficial answer, “I’m fine” doesn’t help anybody. I have picked the best players for my support team, including a fantastic neurologist, nurse and general practitioner – I feel very fortunate.
Putting Things into Perspective
With a diagnosis of MS, you get a quick slap in the face to put things into perspective. Naturally, I felt the immediate desire to make the most of life, be brave, and take imperfect action. I love spontaneous trips away, music gigs, and adventures.
I started consciously practising gratitude. I obviously feel grateful for the general things like health, safety and security. Importantly, I also feel lucky to have subtle reminders of the specific small things that bring joy. I love immersing myself in mindful moments, such as swimming at the beach on a sunny day, flying past on a windsurfer or yacht, or dancing with my kids to loud music. I like to believe that this subjective well-being contributes to my current remission.
Finally, I am learning to put my desire for denial aside by raising awareness about this sometimes invisible MS battle. It is a marathon, not a sprint, but I am not alone.
To other parents going through a similar experience
Whatever health condition you are facing, whether physical or psychological, you are never alone. People want to help and support you. It’s important to stay present and trust that you can cope with difficult things that arise throughout the process. You are more resilient than you think, and you may have strengths you can transfer from other areas of your life. The diagnosis does not define you. Your values and connections are the most important thing.
To follow Sarah’s clinical psychologist page visit: https://www.instagram.com/dr.sarahbellbooth.psych/